A call comes in before the workday has really started. A tenant hasn’t been seen in days. Maintenance opens the unit with law enforcement present, and now you’re standing outside a door trying to make sense of the next decision.
Or maybe it’s a warehouse injury. There’s blood on concrete, a discarded bandage near a drain, and several employees nearby asking if the area is safe to enter.
In those moments, most property managers aren’t wondering about legal terminology. They’re asking practical questions. Can anyone go inside? Does housekeeping handle this? What has to be reported? What if someone gets exposed? What if the cleanup is done wrong and creates a second problem later?
That’s where universal precautions osha becomes more than a compliance phrase. It becomes the rule that helps you slow down, assume risk before you can confirm it, and protect people first. In biohazard settings, that mindset matters because blood and other potentially infectious materials don’t come with labels. The hazard may be obvious, or it may be partly hidden in porous materials, splash zones, HVAC pathways, or discarded sharps.
Property owners and facility managers often discover that their responsibility doesn’t end when the visible scene is cleaned. A poorly handled incident can affect worker safety, site access, insurance documentation, tenant confidence, and future liability. That’s why a crisis response has to start with control, not improvisation.
Responding to a Biohazard Emergency
A common mistake after a traumatic event is treating the scene like a difficult janitorial issue. It isn’t. An unattended death, suicide, severe assault, industrial accident, or medical emergency can leave behind bloodborne hazards, contaminated surfaces, and emotional trauma for everyone involved.
The first pressure usually comes from operations. Someone wants the room reopened. A supervisor wants a quick wipe-down. A resident wants belongings immediately. Those requests are understandable, but they can push people into dangerous decisions.
When a scene may involve blood or bodily fluids, your first job is to control access and avoid adding more exposures. That means no curious staff, no untrained maintenance response, and no assumption that “small” contamination means “low” risk. Respiratory concerns can also matter, especially in enclosed spaces with disturbed materials, which is why understanding airborne risks in biohazard environments helps property teams recognize when the danger goes beyond what they can see.
What the first minutes should feel like
A disciplined response is quiet and controlled.
- Limit entry: Keep people out unless they have a defined role.
- Pause cleanup efforts: Don’t hand a mop, towels, or spray bottle to staff.
- Identify decision-makers: One person should coordinate communication, site security, and vendor contact.
- Protect dignity: If the event involves death or serious injury, keep the area private and avoid unnecessary discussion.
Practical rule: If you don’t know exactly what materials are present, treat the area as contaminated until trained professionals determine otherwise.
That approach protects workers, but it also protects the property owner. Once an untrained employee starts handling contaminated material, your exposure risk changes. So does your documentation problem. Now you may be dealing with employee exposure concerns, disposal issues, and questions about whether proper procedures were followed from the start.
The real issue isn’t speed alone
You do need a fast response. But speed without protocol creates expensive mistakes.
A strong response does three things at once. It protects health, preserves documentation, and reduces the chance that today’s emergency becomes next month’s claim. That’s why universal precautions are the starting point for serious biohazard incidents. They give you a simple instruction under pressure: assume infectious risk first, then act accordingly.
What Are Universal Precautions The Core OSHA Concept
Universal precautions means treating human blood and certain other potentially infectious materials as if they can transmit infection, regardless of whether anyone knows the source person’s medical status. The easiest way to understand it is this: treat every downed power line as live until proven otherwise.
That principle was introduced because waiting for certainty is dangerous. In a crisis, people often say things like “we don’t think the person had anything” or “it was only a small amount.” OSHA’s framework rejects that guesswork.
Where the rule came from
The Centers for Disease Control and Prevention introduced universal precautions in 1985 in response to the emerging HIV epidemic. OSHA then codified those principles in its Bloodborne Pathogens standard, 29 CFR 1910.1030, in 1991, making them mandatory for an estimated 18 million healthcare and at-risk workers. OSHA also notes that worker fatalities fell from about 38 per day in 1970 to 15 per day in 2023, reflecting the broader impact of proactive workplace safety rules, including bloodborne protections (OSHA worker protections overview).
That history matters for property managers because it explains the intent of the rule. Universal precautions weren’t designed for paperwork. They were designed to stop people from making risky judgment calls under pressure.
What materials are covered
Under OSHA’s bloodborne framework, the concern isn’t limited to obvious pools of blood. Universal precautions apply to human blood and specified other potentially infectious materials, often shortened to OPIM.
Examples include:
- Blood and visibly blood-contaminated fluids
- Semen and vaginal secretions
- Cerebrospinal, synovial, pleural, peritoneal, pericardial, and amniotic fluid
- Saliva in dental procedures
- Any body fluid where it’s hard to tell what’s present during an emergency
For many readers, confusion often begins at this point. People hear “universal precautions” and assume it means every body fluid in every context. OSHA’s original concept is narrower than that, but for real-world scene safety, experienced responders often work more broadly because mixed contamination is common and scene details are often incomplete. If you need a plain-language primer on exposure concerns, this guide to common bloodborne pathogens helps connect the rule to the actual risks people worry about after a crisis.
Universal precautions doesn’t ask you to diagnose the person. It asks you to control the exposure.
Why property managers should care
You may not be the person wearing gloves and collecting waste, but you are often the person responsible for the site, the staff, and the decision to bring in the right kind of help.
That makes universal precautions osha a management issue, not just a worker issue.
A property owner who treats a scene casually can create several avoidable problems:
| Situation | Risk created by assumption |
|---|---|
| Sending maintenance to wipe visible blood | Worker exposure and improper waste handling |
| Reopening space too early | Secondary contact by tenants, staff, or vendors |
| Throwing contaminated materials into regular trash | Disposal violations and chain-of-custody problems |
| Letting multiple people enter “just to look” | Expanded contamination area and privacy failures |
The rule is simple because emergencies are not. When blood or OPIM may be present, assume risk first. Then bring the right controls to the scene.
From Universal to Standard Precautions The Evolution of Safety
Universal precautions is still the phrase many people use, especially when discussing OSHA’s Bloodborne Pathogens standard. But modern infection control didn’t stop there. The approach widened because real incidents rarely stay neatly inside one category.
The practical question for a property manager isn’t academic. It’s operational. If your building has a trauma scene, a medical event, an unattended death, or a hoarding environment with bodily fluid contamination, you need to know whether the response should address only bloodborne risk or a broader set of pathogens.
The basic difference
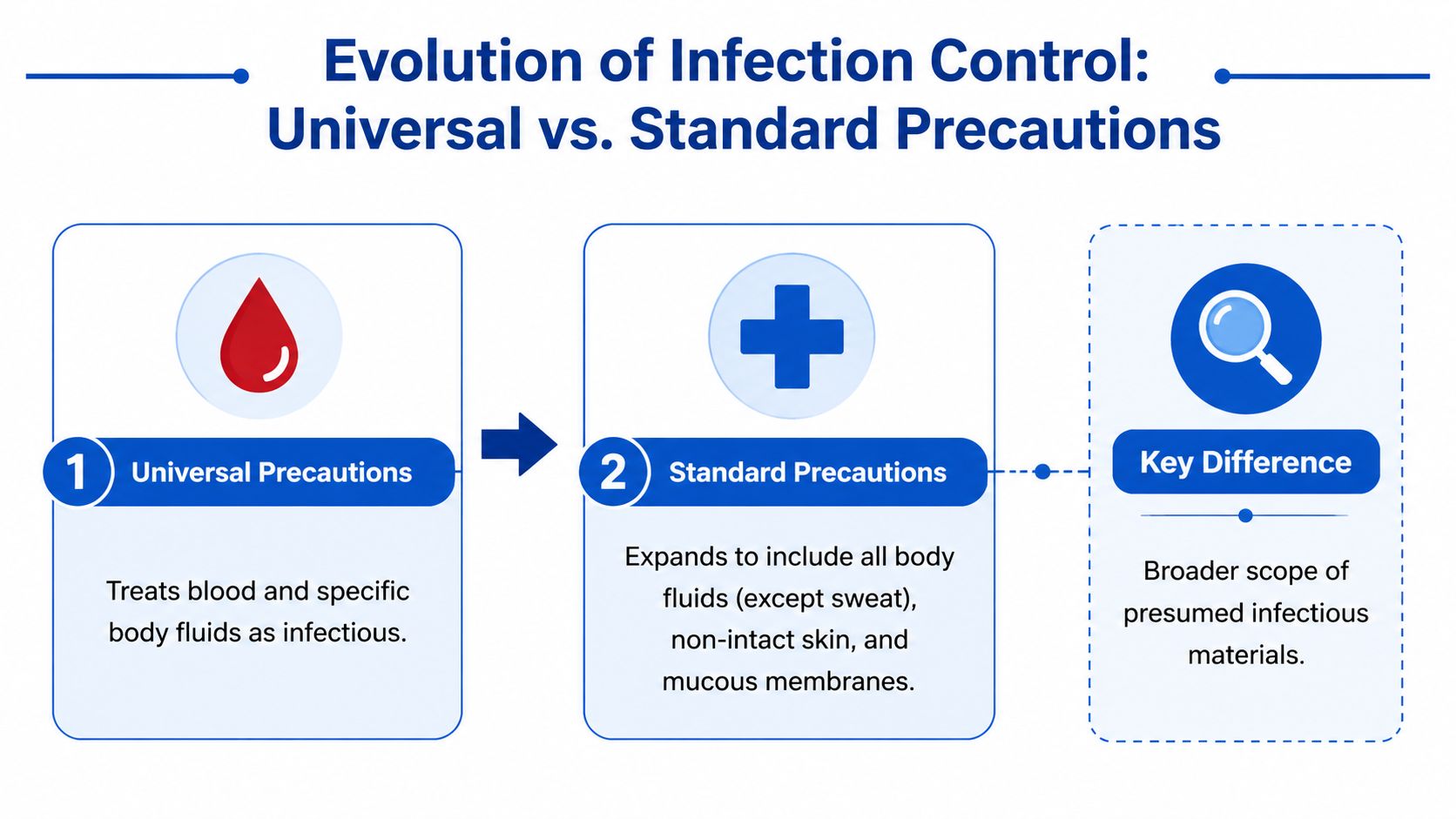
Universal Precautions began as a bloodborne pathogen strategy. It tells workers to treat blood and specified potentially infectious materials as infectious.
Standard Precautions is the broader modern framework. In 1996, the CDC integrated universal precautions into standard precautions, which guide handling of blood, bodily fluids, secretions, and non-intact skin. OSHA data also shows total recordable workplace incidents fell by 78%, from 10.9 per 100 workers in 1972 to 2.4 in 2023, and the same data set attributes prevention of an estimated 99% of preventable accidents in high-risk environments to these broader safety systems (OSHA common statistics).
For a non-clinical reader, the cleanest way to think about it is scope.
Side-by-side view
| Framework | Main focus | What it means on site |
|---|---|---|
| Universal Precautions | Blood and specific OPIM | Assume listed materials are infectious |
| Standard Precautions | Broader body fluid and contact risks | Apply baseline protection more widely |
| Transmission-Based Precautions | Specific route of spread | Add targeted controls for contact, droplet, or airborne concerns |
Why the distinction matters in real buildings
A facility manager may hear “OSHA requires universal precautions” and assume that’s the whole answer. It isn’t always. In a hospital, behavioral health setting, multifamily property, or industrial facility, the scene may involve contaminated surfaces, non-intact skin exposure, respiratory concerns, or mixed waste streams.
That’s why trained teams often work from the more encompassing perspective used in current infection control practice. PPE selection, area containment, disinfection chemistry, waste handling, and room re-entry decisions all depend on understanding the true exposure picture. This is also why the role of PPE in ensuring safety during biohazard cleanup can’t be reduced to “just wear gloves.” Gloves may be the minimum. They may also be nowhere near enough.
A scene can start as a blood exposure issue and quickly become a contact, droplet, or airborne control problem.
Transmission-based precautions add another layer
When a site has pathogen-specific concerns, Transmission-Based Precautions come into play. These include:
- Contact precautions: Focused on preventing spread from surfaces and direct touch.
- Droplet precautions: Used when larger respiratory droplets are a concern.
- Airborne precautions: Used for pathogens that require tighter respiratory control.
This matters in settings where bodily fluids, disturbed materials, confined rooms, or vulnerable occupants increase complexity. A professional response doesn’t just ask, “Is there blood?” It asks, “What else could be present, and what route of exposure matters here?”
What property owners should take from this
If you’re responsible for a site, use this hierarchy as a risk filter.
- Universal precautions is the minimum mindset.
- Standard precautions reflects broader real-world exposure control.
- Transmission-based precautions become critical when the scene suggests contact, droplet, or airborne concerns.
That’s part of the liability shield many property owners miss. A vendor who only addresses what’s visible may leave you with unresolved risk. A response built around broader precautions is more likely to protect staff, occupants, and the property itself.
Your Responsibilities An Employer's Guide to the OSHA BBP Standard
If your employees can reasonably encounter blood or other potentially infectious materials during their work, OSHA doesn’t treat that as an occasional inconvenience. It treats it as an exposure risk that must be managed through a formal system.
For employers, the Bloodborne Pathogens standard is not a suggestion. It sets duties around planning, equipment, training, vaccination access, and post-exposure action. Property managers sometimes assume these rules apply only to hospitals. They don’t. If maintenance staff, security personnel, housekeepers, janitorial workers, or supervisors may face occupational exposure, the standard matters.

Start with a written exposure control plan
Your Exposure Control Plan, or ECP, is the operating document that tells OSHA and your staff how the organization manages bloodborne risk. If you have exposure potential but no meaningful written plan, you’ve already lost control of the situation before an incident occurs.
A workable ECP should identify:
- Which job roles face occupational exposure
- What tasks create that exposure
- Which controls are used to reduce risk
- How training, reporting, cleanup, and follow-up happen
- Who is responsible for maintaining the program
The plan has to reflect what happens on your property. A generic binder on a shelf won’t help when an employee finds contaminated sharps in a stairwell or blood in a restroom after an assault.
OSHA expects a hierarchy of controls
The BBP standard follows a sequence. First reduce the hazard by design where possible. Then control how the task is performed. Then protect the worker with PPE.
OSHA’s BBP standard requires engineering controls, work practice controls, and appropriate PPE. Safer needle devices can reduce injuries by up to 83%, and for decontamination a 1:10 dilution of bleach with a 10-minute contact time is the benchmark for inactivating HBV on surfaces. OSHA also frequently cites improper PPE use as a leading violation (LSU environmental health summary of universal precautions requirements).
Engineering controls
These are physical tools or systems that reduce exposure without relying only on human memory.
Examples include:
- Sharps containers placed where exposure may occur
- Safer sharps devices in clinical settings
- Handwashing stations
- Barrier systems or restricted access controls during remediation
If a worker has to carry a sharp across a room to find disposal, your system has already failed that worker.
Work practice controls
These are rule-based behaviors that make tasks safer.
Common examples include:
- No recapping needles
- Immediate disposal of sharps in puncture-resistant containers
- Handwashing after contact or glove removal
- No eating or drinking in contaminated work areas
- Controlled doffing of PPE to avoid self-contamination
Many employers often fall short in this regard. They provide supplies, but they don’t audit the habits.
Management test: If you can’t describe how an employee safely removes contaminated gloves on your site, your program needs work.
PPE must be provided, maintained, and enforced
Buying a box of gloves doesn’t equal compliance.
Employers must provide PPE that matches the exposure risk. Depending on the task, that may include gloves, gowns, masks, eye protection, or face shields. The equipment must be available where needed, in usable condition, and supported by training on when to wear it, how to remove it, and what to do after contamination.
PPE failures often happen in ordinary ways. Wrong glove type. No eye protection for splash risk. Reaching for supplies after entering the scene. Staff wearing contaminated gear into clean areas. Those failures aren’t minor. They’re how preventable exposures happen.
For teams that need a clearer operational framework, this guide to OSHA guidelines for biohazard exposure and workplace incidents is useful for translating broad requirements into site-level procedures.
Training and vaccination are employer duties
Annual training isn’t optional for exposed employees. Workers need to understand the hazard, the controls, the limits of PPE, and the reporting process after an incident.
The Hepatitis B vaccination series also sits inside the bloodborne pathogen framework for at-risk workers. Employers can’t wait until after exposure to think about that obligation.
A training program should answer practical questions, not just recite regulations:
- What exactly counts as OPIM on this property?
- Who secures the area?
- Where are spill kits and sharps containers located?
- Who authorizes outside remediation?
- What happens if exposure occurs after hours?
This short video is a helpful refresher on the broader OSHA mindset behind exposure control and jobsite response.
Decontamination is not ordinary cleaning
One of the most dangerous assumptions in facility management is that a contaminated area can be “sanitized” by routine custodial methods. Biohazard decontamination requires the right disinfectant, the right dwell time, the right PPE, and the right waste stream handling.
Even when bleach is appropriate, it has to be mixed and used correctly. A 1:10 dilution with a full 10-minute contact time is a benchmark tied to HBV surface inactivation, not a suggestion to spray and wipe immediately.
That difference matters legally. If an employer claims a site was cleaned but can’t show that the method matched the hazard, the documentation may not protect them later.
Why this matters beyond the regulation itself
The OSHA BBP standard forces employers to think like risk managers.
It asks basic but powerful questions. Did you identify exposure-prone tasks? Did you reduce risk before the incident? Did you equip and train people properly? Did you control the cleanup and waste stream correctly? When those answers are weak, liability usually spreads far beyond the original scene.
Actionable Protocol Biohazard Discovery and Cleanup Checklist
A property manager gets a call at 6:10 a.m. A tenant found blood in a hallway bathroom. Maintenance is on site. Housekeeping will arrive in thirty minutes. The first decision matters more than the first mop.
At this stage, your job is scene control. Universal precautions treat the material as potentially infectious until trained personnel assess it. That approach protects workers, tenants, vendors, and the owner’s legal position if questions come later about who entered the area, what was touched, and how waste was handled.

The first-response checklist
Use these steps in the first minutes after discovery.
Secure the area immediately
Close and isolate the space. Lock doors if appropriate. Block access points. In a hallway, lobby, elevator area, or shared restroom, assign someone to keep people back until formal controls are in place. Containment works like a fire door. It limits spread and preserves control.Assess visually from a safe distance
Do not touch surfaces, linens, trash, tools, drains, or personal property. Do not move furniture to inspect the edges. A hands-off assessment is enough for the initial report.Assume the visible area is smaller than the actual hazard
Fluids can soak into grout, subflooring, fabric, seams, baseboards, and porous materials. What you see on the surface may be only the top layer of the problem.Identify immediate hazards
Look for sharps, broken glass, used medical supplies, bodily fluids, damaged surfaces, or signs that air handling could spread contamination. If the scene involves discarded needles or contaminated debris, follow procedures for biohazard waste disposal and regulated waste handling rather than ordinary trash removal.
If body fluids are present, assume the risk may extend beyond the obvious stain line.
Match the response to the exposure risk
Some scenes involve more than bloodborne pathogens. A person who vomited in a confined room, a space affected by heavy waste accumulation, or an area tied to respiratory illness may require precautions for contact, droplet, or airborne transmission.
That distinction matters for owners and facility managers because it changes who can enter, what PPE is needed, and whether ventilation must be controlled before work starts. A dust mask and basic gloves are not a substitute for a trained assessment. The CDC NIOSH training module on precautions and respirator programs explains how respiratory hazards can require fit-tested respirators and a formal program, not improvised PPE use (CDC NIOSH training module on precautions and respirator programs).
Who to notify and what to record
Once the scene is stable, start the administrative response. This step is part safety control and part liability control.
Notify the right people
Your chain of communication may include:
- Property ownership or site leadership
- HR or employee safety personnel
- Risk management or legal contact
- Insurance carrier or claims contact if coverage may be affected
- Qualified remediation provider
- Local authorities, if the circumstances require law enforcement, EMS, or coroner involvement
A delayed notification can create the same kind of problem as a delayed water shutoff after a pipe break. More people enter. More materials are affected. More questions follow.
Document without disturbing the scene
Good records reduce confusion and help show that the site was handled responsibly from the first moment of discovery.
Record:
- Time and date of discovery
- Name of the person who found the scene
- Exact location and areas isolated
- Who was notified and when
- Whether anyone entered, touched materials, or attempted cleanup
- Visible hazards such as blood, sharps, bodily fluids, or damaged finishes
- Photos taken from a safe distance, if your policies permit
Keep the notes factual and brief. Do not speculate about medical history, cause of death, fault, or what “probably” happened.
What not to do
Early mistakes often create the largest liability trail.
- Do not send janitorial or maintenance staff into the scene unless they are trained, equipped, and authorized for that exposure risk
- Do not place contaminated waste, linens, PPE, or sharps into regular trash
- Do not allow residents, tenants, staff, or family members to retrieve belongings before clearance
- Do not turn fans, reopen HVAC zones, or use vacuums and floor machines before spread risk is assessed
- Do not treat odor control products as proof of decontamination
- Do not rush disposal decisions if you want to avoid penalties for hazardous waste
Speed without protocol creates expensive mistakes.
The handoff to a professional cleanup team
After containment, notification, and documentation, the next phase is technical remediation. That usually includes a hazard assessment, PPE selection, controlled removal of affected materials, cleaning and disinfection, verification, and compliant packaging and disposal of waste.
Your role is closer to an incident commander than a cleaner. You set the perimeter, control access, document decisions, and keep untrained people out of harm’s way. That is how universal precautions function as more than an OSHA rule. They become a practical risk-management system that helps protect the property, the people on site, and the owner’s position if the cleanup is examined later.
Beyond Compliance The Hidden Liabilities of Improper Cleanup
A visible stain can be removed quickly. Liability usually can’t.
That’s the problem with treating biohazard response as a cosmetic cleanup issue. If contaminated materials were handled incorrectly, if staff entered without proper controls, or if waste left the site through the wrong channel, the legal and financial consequences can continue long after the room looks normal again.
Where property owners get exposed
OSHA focuses on worker safety, but property owners often face the downstream effects. The available guidance also points to a rise in claims tied to improper hoarding and trauma cleanups, and some data suggests a 25% increase in OSHA citations for improper sharps disposal in non-medical sites. The same guidance notes serious violations can average $14,000 in fines, which is one reason insurers and owners pay close attention to how a scene was handled (OSHA interpretation context on downstream compliance issues).
That doesn’t just mean OSHA citations. It can mean a denied claim, a dispute with a tenant, a complaint from a future occupant, or questions from counsel about why untrained employees were put into the scene.
The liability gap most people miss
Many owners think the main risk is an enforcement action. Often the bigger problem is documentation.
If a cleanup was informal, you may not have:
- A clear record of when the area was secured
- A log of who entered the scene
- Proof of what materials were removed
- Evidence that waste was handled through the correct stream
- Support for the insurance file
That gap becomes painful when a carrier asks for records, when an employee reports an exposure concern later, or when a buyer, tenant, or regulator asks what was done.
If you’re reviewing your obligations around regulated disposal and want a plain-language overview of how organizations avoid penalties for hazardous waste, that guidance is useful alongside site-specific biohazard procedures.
Improper cleanup doesn’t stay contained. It spreads into HR, insurance, leasing, operations, and reputation.
The human cost is often ignored
There’s another liability that doesn’t always appear on a spreadsheet. Asking untrained staff to clean a traumatic scene can cause lasting distress.
A porter, housekeeper, leasing agent, or maintenance technician didn’t sign up to process a death scene, collect bodily fluids, or make judgment calls about contaminated personal belongings. Even if that person says yes in the moment, the impact can surface later as anxiety, anger, absenteeism, or a sense that management abandoned its duty of care.
That’s one reason careful owners separate emergency scene control from ordinary housekeeping. Specialized cleanup exists because the hazard is technical and the event is often traumatic.
For teams building stronger procedures around regulated removal and final handling, this overview of biohazard waste disposal helps connect the cleanup decision to the waste stream decisions that follow.
Your Partner in Safety and Recovery
Universal precautions osha gives you the baseline rule. Treat blood and defined infectious materials as hazardous from the start. That mindset prevents dangerous guesswork and creates order when the scene is chaotic.
For property owners and facility managers, though, the bigger lesson is this: minimum compliance is not the same as full risk control. Real incidents often involve broader contamination concerns, documentation demands, worker-protection duties, occupant sensitivity, and disposal requirements that ordinary cleaning programs weren’t built to handle.
That’s why the safest response is usually the most disciplined one. Secure the area. Limit entry. Document facts. Protect staff from being pulled into tasks they aren’t trained for. Then move the incident into a professional remediation process that addresses both health risk and liability.
At 360 Hazardous Cleanup, we see these events through both lenses. Safety and human impact. A site has to be handled in a way that protects workers, respects families and occupants, and stands up to scrutiny later. When a crisis hits, the right response gives you more than a clean room. It gives you a defensible process and a path back to normal operations.
Frequently Asked Questions about Biohazard Safety
| Question | Answer |
|---|---|
| What does universal precautions osha mean in plain language? | It means you treat blood and certain potentially infectious materials as if they can transmit infection, even when you don’t know the source person’s status. |
| Can my regular janitorial team clean blood after an incident? | Only if the employer has properly addressed exposure risk through training, equipment, procedures, and oversight. Many serious incidents need specialized remediation rather than routine custodial work. |
| Is visible cleanup enough to reopen a room? | No. Visible soil removal is only one part of the response. Surface contamination, porous material impact, waste handling, and safe re-entry all matter. |
| Do property managers have liability even if OSHA doesn’t cite them? | Yes. Insurance, employee exposure concerns, tenant complaints, and future occupancy issues can all create downstream risk. |
| Why is documentation so important? | It helps show when the area was secured, who responded, what hazards were present, and how cleanup and disposal were handled. That record can matter in claims and internal reviews. |
| When should I call a professional biohazard team? | As soon as you identify a scene involving blood, bodily fluids, sharps, trauma, unattended death, or uncertain contamination. Early control usually prevents bigger problems later. |
If you need help after a trauma scene, unattended death, industrial accident, or other biohazard event, contact 360 Hazardous Cleanup. Our team is available 24/7 to help you secure the site, guide through the next steps, and move the property toward safe, compliant recovery with discretion and care.


